COVID-19 has opened the door to more widespread health monitoring, but sensors are getting more complex and testing isn’t always easy.
Now that COVID-19 pandemic has desensitized us to telemedicine and more at-home health monitoring, the way we receive health care probably has changed for good. The no-touch thermometer and our personal pulse oximeter are not just coveted gadgets now. They have true clinical use in what may become a “point-of-use” system. Point of use means we don’t have to go to the clinic to get screened.
But how are sensors being readied for this new role? Are they accurate enough?
Testing sensors during and after production-level manufacturing is not like testing digital integrated circuits. While digital circuits are in sensors and get tested as such, sensors often have analog components that need calibration as well as testing. On top of that, sensors are getting more complex. With multiple sensor types working in the same small form factor, the complexity of design and testing goes up.
The challenge in testing sensors isn’t about typical issues in advanced nodes. “You don’t really have that problem,” said Andrew Baker, managing director of Maxim Integrated’s Industrial & Healthcare Business Unit. “With these devices in the analog world, we are talking about 0.18 micron, moving to potentially 90nm.”
The bigger issue, said Baker, is designing sensors at the system level to get sufficient accuracy and good SNR (signal-to-noise ratio) out of a sensor. COVID-19 is really bringing home that lesson as different companies are attempting to design a handheld COVID testers. “It’s really at a system-level design that you need to consider,” said Baker.
On one level, system design means all these sensors can maintain their accuracy together in small form factor, which someday could be as thin as a body-worn patch, without being too power hungry. The COVID testers will monitor key vital signs:

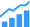
Fig. 1: Maxim Integrated’s typical application circuit for the MAX30002 ECG AFE. Source: Maxim Integrated
Mixing it up
The mix of sensors is supposed to guard against false positives. You don’t want to think you have COVID-19, when you only have a cold. “Temperature is becoming very, very critical these days. We want to look at trends. Is somebody getting a fever or is it just hot? There needs to be some context to all of this and hence the desire to have multiple sensing modalities in a device so that they will have to correlate,” said Baker. “It’s almost like an ejector seat. Don’t eject the guy unless three computers concur.”
Having a mix of sensors, algorithms and some computing power is necessary.
Other sensor types are worth looking at. “Optical which is a huge area. It is very convenient, it’s noninvasive, it’s widespread and easy to deploy and there’s a lot of development going on that area, both from a hardware as well as algorithms and software. SpO2, of course, is the method you would use optical to measure,” he notes.
A new emerging area is electrochemical. “We announced our first product in the electrochemical area really targeted toward continuous glucose monitoring (CGM),” said Baker. “This is an area of development. Basically, you can categorize it into fluidics. It could be in vitro, so that it was measuring stuff in the blood in the body. In the case of CGM, it’s a minimally invasive sensor that’s inserted a couple of millimeters below the skin. And then you’re basically looking for a chemical reaction there with the glucose, in the actual interstitial fluid. But this is the area that could be developed in terms of point-of-care and point-of-use devices — anything you can measure electrochemically. It could be an antibody or any kind of fluid that you want to see the content in electrochemical way.”
Gas sensors are a frontier for health that you don’t see as often — yet. But they do have potential in the health care field, as well as in environmental sensing. Checking “out breath” — the gas composition of a person’s breath — has relevance to diabetes for certain, and perhaps other diseases.
“If a person has a very bad digestive disorder, the composition of breath will be very different from a person with a healthy digestive system, for example,” said Sreeni Rao, senior director in TDK’s gas and environmental sensing products and business. “Higher levels of acetone — the gas called acetone — in a person’s breath is a clear marker of diabetes. There are lots of instruments that actually make use of that fact that just aren’t as optical as pricking your finger and getting a diabetic reading or blood sugar reading. So that is another angle to this whole breath sensors are our gas sensors. That is also extremely important. What we breathe out has an extremely high medical value.”
But gas sensing has some hard limits. “For inert gases for carbon dioxide, the number of avenues for innovation are actually fairly limited,” Rao said. “But if you take an active gas, like alcohol, they are complex molecules. They are not easy to make react, but they are still active in the sense they react with some chemical. But the electrochemical has to be specific to the gas. It is possible, and there are companies that have products out there that do this kind of reaction with these gases.”
TDK isn’t alone in this endeavor. Arm has developed an organic FET — a plastic armpit sensor — that responds to organic compounds such as body odor. “If you put an array of these devices and add machine learning, it can classify smell as one of the features,” said John Biggs, Arm co-founder and R&D consultant engineer.
Algorithms pick up the signal slack
Perhaps the bigger deal is that algorithms shipped with sensors are almost more powerful than the sensors themselves. Some algorithms are now so good that they can interpret weak signals and make up for the accuracy of a sensor. “You’d be amazed how effective some of these algorithms are getting,” said Baker. “There’s always a challenge in getting a good signal but you can actually extract good amounts of information from a relatively poor signal if you have a very, very good algorithm.”
Algorithms aren’t just for medical sensors, either. They are being used in drug development and testing, as well. Health changes in drug trials need to be measured more effectively and more quickly, and that needs to be fed back into the drug creation pipeline. In effect, one becomes an extension of the other, almost like a biological version of hardware-software co-design.
“The challenge is how you can design drugs that don’t fail as much,” said Guido Lanza, president and CEO of Numerate, a startup focused on molecule chemical design. “When most people think of machine learning, they think of what companies are doing with images. That’s fairly direct mapping to medicine. With AI pattern recognition you can determine where a drug will not work.”
The key here is data, and each data point is expensive and hard to collect, said Lanza. “The way pharma has done this is to try a drug against millions of targets, but that creates a couple of problems. First, it’s not a smart way to do it and second, not everything is testable.”
What isn’t testable can be extrapolated, and then the test equipment can be adjusted. But that requires good data. Once that data is collected, whether locally within a device, or in the cloud, it can be cleaned up and data extracted.
Algorithms also can help to minimize noise. “The biggest confounder in these measurements is really motion,” said Baker. “You’ll have at least the accelerometer gyro in the system. Using that, together with the optical data, you correlate what is the motion and what is the actual heart rate from the signal. The algorithm discerns the signal of interest.”
The question then is whether that signal is accurate. “You need to calibrate temperature and stress with MEMS devices,” said Carl Moore, yield management specialist at yieldHUB. “But these devices also have power management ICs in them, and a lot of the nodes in there are not testable. As you design these devices, you need to understand what are the testable nodes. There may be hundreds of test nodes internally. If you’re testing internal nodes, you decide whether you’re going to run them slow, average, or whether to amplify them to a reasonable level. Or you have to make the design so you can sense it from the outside.”
Noise can crop up from other ambient conditions, as well, including both heat and light. System designers have to take all of this into consideration.
“It really is a system-level design, so if you’ve got a very poor optical architecture, you’re going to get a poor signal,” said Maxim Integrated’s Baker. “No matter what you do with it from the backend electronics, you’re going to get a poor signal. There’s a balance between getting the best signal and having the lowest power. You basically want to have the lowest possible power but get the best possible signal, and then that comes down to how well your algorithm is able to discern those signals. Some algorithms are better at discerning the signal from a poor signal.”
Regulations are your friend
Regulatory approvals mean a lot to health care monitoring system, like a wearable or hearable. The device can legitimately be called ‘clinical grade’ and will be used by doctors more often. Clinical grade lends a certain amount of trust to the results of a monitoring device. The approvals can also put issues in the fore front.
“Because gases are usually invisible — out of sight — they are often out of mind,” said TDK’s Rao, “Consumers needed to be educated that carbon dioxide and carbon monoxide are silent killers. Somebody had to pass regulations — the government in this case — before the carbon dioxide / carbon monoxide sensor market really took off.”
When obtaining FDA or other regulatory approval, it is good to have all the big companies go first through the process. “It’s good that the 800-pound gorilla is paving the way for the other guys to come through. That will benefit the whole market,” said Baker. Once the first device of its kind gets FDA approval, through the de novo process for new devices, other device approvals go through an easier process if its provable that the product is the same.
“We’re now seeing that consumer companies getting FDA approval,” said Baker. “For example, Apple with the Apple Watch. They got FDA approval for afib screening detection. Actually, a lot of those devices are being recommended by doctors. Even the clinicians are seeing value in this. Now that the devices are being FDA approved it really represents the efficacy of these devices and the reliability of the data that’s being provided.”
Testing, calibration costs
Production deployment will have to be ramped up if devices take off. And testing is still costly. “One big contributor to the cost in any MEMS device, not just gas sensors, is really the testing. The big challenge that anybody in the space of gas sensors wants to solve or needs to solve is really the testing cost and testing methodology of testing process,” said Rao. Testing sensors and calibrating them is about putting them in hot baths of oil, chambers with gas pumped in, arms that rotate the sensors against Earth’s gravity, and many more. It all depends on the sensor.
Pretty much every sensor must be tested, too. “You have some of the performance parameters can be guaranteed by design, some can be guaranteed by characterization, but there is a set of parameters on a spec sheet data that you would have to test on a device-by-device basis that would let you bin your devices properly to create a class A, class B, class C,” he said. “There are at least a minimum set of parameters like a basic level of accuracy of gas sensors — how much ppm, how sensitive is it, or how accurate is it? Those kinds of things you cannot avoid testing every device that you produce.”
That also adds to the overall cost. “The testing cost is more than it used to be,” said yieldHUB’s Moore. “There might be 2,000 to 3,000 tests on a device. With digital, you can do highly parallel tests. But with analog, it’s not as easy. For power and MEMS, there is an inherent challenge. You may get 8 or 16 pieces tested at once, but not everything.”
Again a full systems view and design-for-test philosophy will me the difference between success and failure. “When it comes to sensor design–and design of complex systems in general from my point of view test should be implemented from the very beginning,” said Benjamin Prautsch, group manager of Advanced Mixed-Signal Automation at Fraunhofer Institute for Integrated Circuits IIS Division Engineering of Adaptive Systems EAS. “This means we have to take care of testability in general:
Testing and calibration in the sensor market can really pay off in other ways. “We recently introduced a clinical-grade temperature sensor. It’s basically a digital thermometer,” said Maxim Integrated’s Baker. “We have very high level of accuracy out of the factory, so we calibrate this device to 0.1° C. We guarantee that level of accuracy even after the customer has soldered that on their board. Due to mechanical stresses, then temperatures could shift, especially when you solder something on the board. This is generally mechanical stresses. We give some recommendations on how you should solder. Once those recommendations are followed, then we guarantee the accuracy even after it’s been placed on the board. Obviously at the factory it’s more accurate than we guarantee, because there’ll be a slight shift when you put it on the board. The value proposition of this is really super low power for continuous measurement, half the power of our nearest competitor. It’s a 2mm x 2mm package, very tiny, and it has very fast response time in terms of the response to change in temperature.”
Conclusion
The result of the COVID-19 pandemic is more health care will be managed remotely, at home using monitoring devices and telemedicine. It is a genie that COVID has let out of the bottle, and it may help save lives and health care costs.
“I believe this is a shift, not just a temporary blip,” said Baker. “There’s a long-term residual effect of that. Once devices have been deployed, you put that infrastructure in place and it then can be used for the broader population.”
—Ed Sperling contributed to this report.
Leave a Reply